IS BREAST AUGMENTATION WITH MY OWN FAT SAFER AND MORE EFFECTIVE THAN BREAST AUGMENTATION WITH IMPLANTS?
Recently, plastic surgeons as well as other physician providers have begun offering fat grafting as an alternative to breast implants for breast augmentation. This technique, more popular in Japan and some parts of Europe but gaining popularity in the United States, holds promise but is not well-studied and quite controversial.
Currently, the American Society of Plastic Surgeons (ASPS) supports the use of fat grafting for improving contour after breast reconstruction, but does not endorse its use in cosmetic breast augmentation. Click here to read the official position statement from the ASPS and the American Society for Aesthetic Plastic Surgery (ASAPS). Unfortunately, in some cases, the potentially attractive real and theoretical benefits of fat grafting have been marketed to the public without disclosure of the potential problems of this technique and how they could affect breast health.
Fat-Grafting
Some information that should be taken into account when considering fat grafting as an option for breast augmentation includes:
Can my own fat transferred into my own breast still cause breast cancer?
What are stem-cell enriched fat transfers? Are they effective? Could they be dangerous?
How is fat grafting for breast augmentation performed?
How effective is fat grafting for breast augmentation?
1. Can my own fat transferred into my own breast still cause breast cancer?
The short answer is that we don’t know and that’s the problem. There have been no rigorous studies in humans to prove or disprove that this could happen. Doctors who have expressed concern that your own fat when transferred to your breast could become cancer point to several issues. One is that in some animal experiments, transferred fat can be induced to become a cancer but at this point it is in an environment that does not closely resemble what actually happens in humans. Second, more than 10% of women will develop a breast cancer in their lifetime. This would suggest that there are cells in a significant percentage of women’s breasts that could be tipped from a normal state to a cancer-inducing state. Certain female hormones and other naturally occurring chemicals that exist in fat may be able to throw these vulnerable breast cells into a cancerous state. Some doctors are concerned that adding more fat – even your own – to the mix may be enough to induce or speed up the development of a breast cancer. There are no clear data to prove or disprove this.
No. Fat grafting can affect mammography. Injected fat can lead to the development of calcifications, cysts and a redistribution of the breast tissue.
Breast implants will also affect mammography by redistributing breast tissue and making a small percentage of the breast tissue more difficult to image. To get around this, a mammographer will perform additional views called displacement views. The implant is pushed out of the way, the images are retaken, and additional breast tissue, previously hidden, can be imaged. An alternative approach is to perform a screening breast MRI. Since breast implants have a much longer track record, protocols to improve breast imaging after implant-based augmentation are well-developed. By contrast, recommendation and techniques to improve breast imaging after fat grafting are not as well developed because the mainstream application of fat grafting for breast augmentation has not been around as long.
Frankly, any surgical procedure on the breast will affect breast imaging to some degree because the breast has been transformed in some way. A breast reduction, for example, will also cause calcifications, cysts and a redistribution of breast tissue.
3. What are stem-cell enriched fat transfers? Are they effective? Could they be dangerous?
Fat transfers can be enriched with stem cells. Normal fat contains a small fraction of adipose-derived stem cells. Like other stem cells, these adipose-derived stem cells can be manipulated to mature into other cell types. They are affected both by chemicals that already exist in our body, or that can be added to the body as a drug.
The fact that stem cells can change into other cell types is both a good and a bad thing. The good thing is that these cells can help to regenerate missing tissues to either replace missing tissue or augment existing tissue. This is potentially an extremely powerful tool as we reconstruct patients who have had cancer or whose bodies have undergone the natural aging process. Unfortunately, stem cells may also be transformed into rapidly dividing cancer cells.
The major challenge in dealing with these stem cells is control. Scientists need to develop reliable and practical methods for safely inducing stem cells into useful regenerative cells rather than cancer cells. It is not enough for the body to naturally regulate these cells. Cancers clearly form despite the body’s attempts to naturally regulate these cells. So, by the same token, doctors need a reliable means of regulating stem cells to ensure that they are doing what they are supposed to do – helping patients - rather than what they are not supposed to do – creating or worsening a cancer.
New technology has been developed to increase the percentage of stem cells in harvested fat with the hopes that these stem cells will improve the take and effectiveness of fat transfers. Early studies with these devices are under way in Asia.
Despite some premature marketing that has focused on the potential benefits of stem cell-enriched fat transfers, they are still being investigated for their safety and effectiveness and therefore remain experimental. Certainly, if rigorous evaluation concludes that stem-cell enriched fat is shown to be safe and effective, it may one day become a valuable tool. As more information becomes available on this topic, we will update this essay, our blog and Twitter pages.
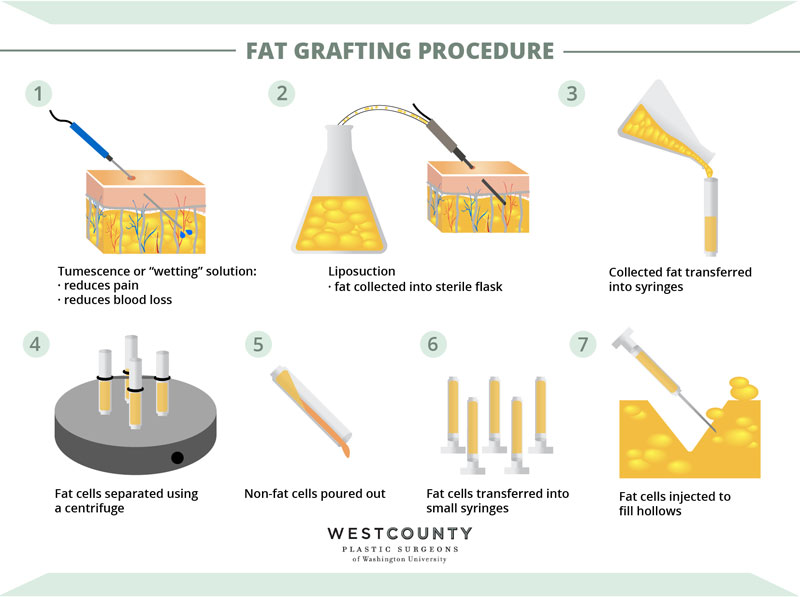
4. How is fat grafting for breast augmentation performed?
Fat is harvested from areas of fatty excess such as the abdomen, flanks and thighs using liposuction and then reinjected into the breasts. The methods of liposuction used for fat harvest and processing of the fat cells after harvest vary and there is no clear consensus or scientific data to convincingly show what works best. The incisions used to harvest and reinject the fat are less than 1 cm. The procedure can be performed with the patient under local or general anesthesia. Some protocols recommend the use of an external breast splint that is worn for several hours a day for several weeks to provide a more conducive environment for fat graft take.
5. How effective is fat grafting for breast augmentation?
Protocols for safe and effective fat grafting for breast augmentation are still being developed. At this time, fat grafting for breast augmentation seems to be most effective for small- to moderate-sized breast augmentations. There is significant variation on how much of the grafted fat stays over time with reports ranging from 30-80%. Repeat sessions of fat grafting may be used to help retain the volume of grafted fat or to produce a larger breast augmentation.
The difference between fat grafting for breast augmentation and breast reconstruction is that in breast augmentation all of a women’s breast tissue is present. Because 10-15% of women will develop a breast cancer during their lifetime, this means that 1 in 8 women who undergo this technique will have cells in their breast that at some point will become cancer cells. By contrast, a woman who has had her breast removed for breast cancer has almost no breast tissue left. Breast reconstruction uses an implant or non-breast tissue to reconstruct the breast.
So, women undergoing fat transfer for breast augmentation have a much higher chance of having breast cells susceptible to becoming a cancer than women who have already had their breast removed. If it turns out that fat grafts can induce breast cancer in breast cancer-susceptible cells, then the breast augmentation patients will be at greater risk.
If you have questions or would like to book a consultation with one of the surgeons at West County Plastic Surgery, please call (314) 996-8800.